For Patients
 Your physician has requested intraoperative neurophysiological monitoring (IONM) for your upcoming head, neck or back surgery. During the procedure, a Quantum Neuromonitoring-trained neurotechnologist (NT) will:
Your physician has requested intraoperative neurophysiological monitoring (IONM) for your upcoming head, neck or back surgery. During the procedure, a Quantum Neuromonitoring-trained neurotechnologist (NT) will:
- Act as your “electrician” and monitor electrical impulses in the nerve structures affected by your surgery.
- Provide an early warning to your surgeon should any potentially harmful changes occur.
- Help prevent any permanent damage to the nervous system from the operation.
If you are a patient facing surgery (or you know someone having surgery), the information and animations in this section will help you understand how IONM can reduce the risk of injury to the nervous system during a surgical procedure.
INTRODUCTION TO IONM
Quantum Neuromonitoring provides a service called intraoperative neurophysiological monitoring (IONM). During head or spinal surgery, a specially trained neurotechnologist (NT) from Quantum Neuromonitoring will continuously monitor (or check) your nervous system. The NT monitors the electrical impulses as they pass through the spinal cord to the brain throughout the surgical procedure. The purpose of IONM is to reduce the risk of injury to the nerve structures directly involved with the type and location of your surgery.
IONM helps to make your surgery go smoothly by:
- Allowing the NT to let the surgeon know immediately if there are any negative effects observed which could interfere with the function of your spinal cord or neural structures.
- Enabling the NT to work closely with your anesthesiologist to monitor how the anesthetic agents administered interact with the nervous system.
- Reducing many of the risks involved with surgery, and increasing the chance of a successful outcome.
For example, studies have shown that with the use of monitoring in surgeries such as correction of a scoliotic deformity, neurological deficits can be minimized.
You can be assured that your safety is our primary concern at Quantum Neuromonitoring. The NT involved with your surgery is highly trained and experienced in using IONM and is considered an integral part of the surgical team.
MONITORING YOUR SURGERY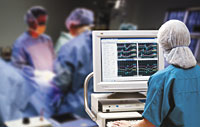
Prior to your surgery, the neurotechnologist (NT) who will conduct intraoperative neurophysiological monitoring (IONM) during your procedure will meet you in the preoperative holding area. After obtaining pertinent
information from your chart, the NT will attach multiple surface electrodes to stimulate the nerve structures involved with your procedure. The number of electrodes used and the placement of these electrodes is dependent upon the type of surgery you are having. Tape is used to secure the electrodes carefully, because once the procedure is underway, it is difficult and sometimes impossible for the NT to add more electrodes.
When you are brought into the operating room:
- The electrodes will be attached to a biomedical computer designed specifically for the purpose of intraoperative monitoring.
- You will be anesthetized and positioned on the operating room table.
- Sterile, disposable needle electrodes will be inserted under the skin of the scalp and along the nerve structures to record responses obtained from the stimulating electrodes.
Before the surgery begins, the NT makes a baseline recording of all the nerves involved and stores the information for comparison to subsequent recordings. Depending on the length of your surgery, any combination of the nerves monitored may be stimulated several thousand times. These stimulations are mild and will not cause injury to the nerves themselves.
When your surgical procedure has been completed, but before you recover from anesthesia, all stimulating and recording electrodes will be removed.
 How Monitoring Works
How Monitoring Works
The NT will notify the surgeon if the latency (or time frame) of the response changes by 10 percent or the amplitude (or intensity) of the response decreases by 50 percent. For example, the evoked response obtained with stimulation of the tibial nerve at your ankle may take 40 milliseconds to reach the brain. If this response were to increase by four milliseconds when compared to your baseline recording, the NT would have sufficient cause to notify the surgeon of this change. The amplitude and latency of a response equal each other in importance.
A change in amplitude may occur independently of a change in latency, or they may happen at the same time.
Additional modalities (or diagnostic tests) used during monitoring may include:
- Monitoring of the electromyographic response (or motor activity) produced by irritation of a nerve that can cause the muscle to contract (called spontaneous electromyographic activity).
- Electrically stimulating an implant such as a pedicle screw used to stabilize the spine to ensure the implant has been placed in the proper position (called triggered electromyographic activity).
- Monitoring of blood oxygen saturation (SPO2) from the big toe to see if blood flow to the lower extremities decreases (as with anterior lumbar surgery).
We are capable of stimulating the motor cortex of the brain and recording responses from appropriate muscle groups. This technique proves very valuable in corrective surgeries such as the reduction of a scoliotic deformity. The NT checks both motor evoked potentials (MEPs) and somatosensory evoked potentials (SSEPs) during this procedure. MEPs monitor the motor pathways located in the front of the spinal cord, while SSEPs monitor the sensory pathways located in back of the spinal cord.
